 80314388
80314388
Diabetes and Trigger Finger: What You Should Know

Summary:
- If you have diabetes, you may be at risk for trigger finger, a condition where your finger catches, clicks, or locks when you bend it.
- Early awareness is key — recognising stiffness, popping, or locking allows you to take action before pain or long-term stiffness develops.
- Managing your diabetes, and working with an orthopaedic specialist can prevent complications, restore hand function, and improve long-term outcomes.
If you have diabetes, you could be at risk for trigger finger, a condition where a finger catches, clicks, or even locks when you bend it. It’s more common than many people realise, and early awareness can make a big difference.
Keep reading to learn how diabetes can impact your tendons and discover simple ways to protect your hands and keep them moving smoothly.
How Diabetes Increases the Risk of Trigger Finger
Diabetes can change the way your tendons function, making them more prone to irritation and thickening. Here’s how high blood sugar affects your hands and what makes some people more at risk.
Why High Blood Sugar Affects Tendons
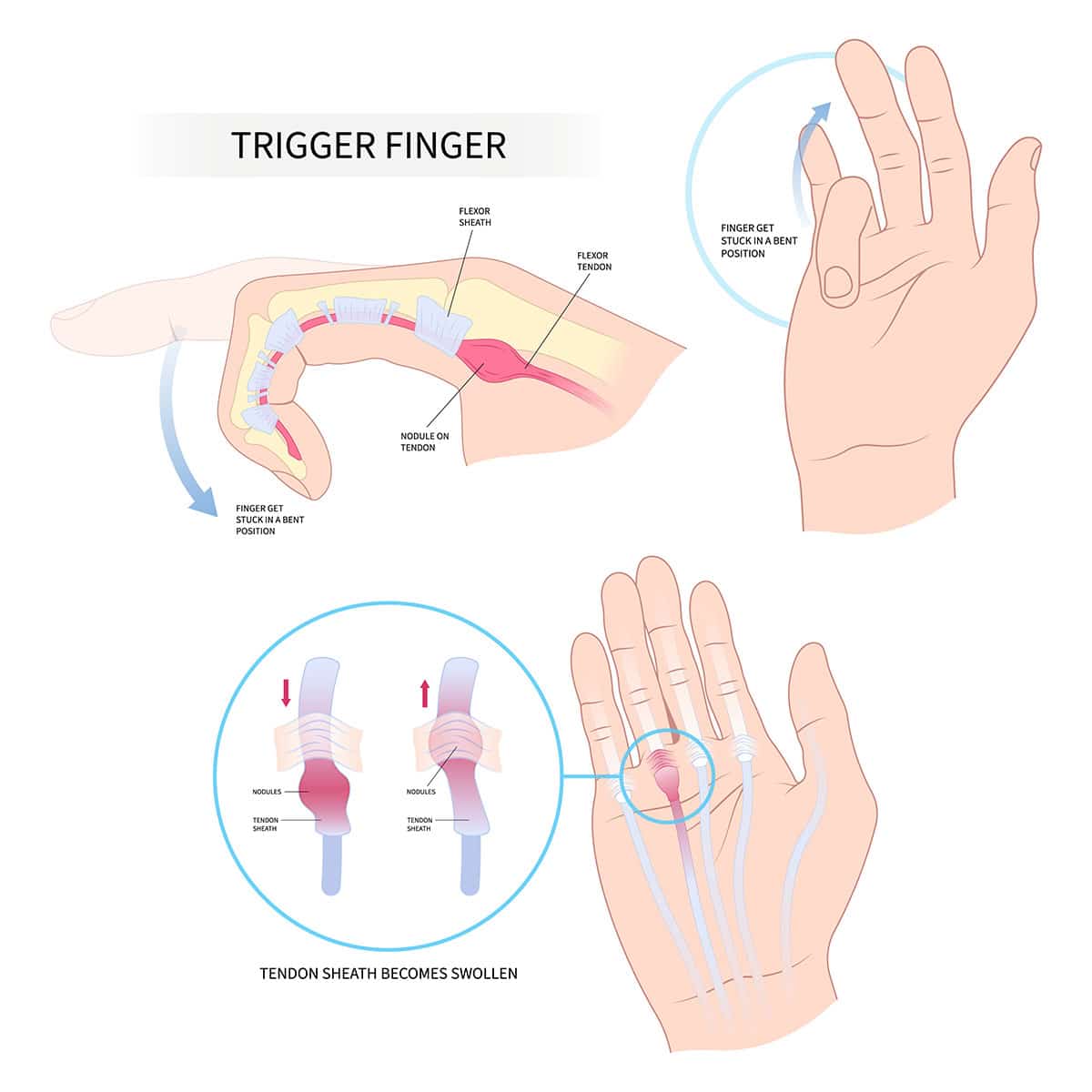
High blood sugar over time can damage small blood vessels and tissues, including the tendons in your hands. This can cause the tendon sheath — the protective covering around your tendons — to thicken or stiffen, making it harder for your tendons to glide smoothly. The result is fingers that click, lock, or feel stiff.
Common Risk Factors in Diabetic Patients
Not all people with diabetes develop trigger finger, but certain factors increase the risk: long-standing diabetes, poor blood sugar control, and other complications like neuropathy.
Age, gender (more common in women), and repetitive hand use may also play a role.
Early Signs and Prevention of Trigger Finger
Catching trigger finger early makes a big difference. Here’s what to look for and simple steps to reduce your risk.
Recognising Stiffness, Clicking, or Locking in the Fingers
Watch for early warning signs: fingers that feel stiff in the morning, clicking or popping when you bend or straighten them, or a finger that locks in a bent position. Noticing these symptoms early allows you to take action before the problem worsens.
Exercises and Habits to Reduce Risk
Simple hand stretches and tendon-gliding exercises can keep your fingers flexible. Avoid prolonged gripping or repetitive motions without breaks, and maintain good blood sugar control — both are key to protecting your tendons.
Managing Diabetes and Trigger Finger
Managing your diabetes is a key part of managing trigger finger. Controlling blood sugar helps reduce tendon stress and keeps your fingers moving smoothly.
Blood Sugar Control and Its Role in Hand Health
Keeping your blood sugar within target ranges reduces stress on your tendons and can help prevent trigger finger from worsening. Work with your doctor to monitor your levels and manage diet, exercise, and medication.
When to Seek Medical Advice
If your finger becomes painful, locks frequently, or interferes with daily tasks, it’s time to see an orthopaedic specialist. Early assessment allows for non-surgical treatments and helps prevent permanent stiffness or deformity.
At Spire Orthopaedic Centre, we have experience helping patients in Singapore with trigger finger and can provide advice tailored to your health needs. Book a consultation today.
Treatment Options Safe for Diabetic Patients
There are safe and effective ways to treat trigger finger, whether with conservative measures or surgery. Here are some to consider.
Non-Surgical Approaches (Splints, Physiotherapy, Steroid Injections)
Most trigger fingers can be managed without surgery.
Splints can rest the affected finger, physiotherapy helps maintain motion, and steroid injections can reduce inflammation. These treatments are generally safe for people with diabetes, though your doctor may monitor blood sugar after injections.
Surgical Options and Considerations for Diabetic Patients
If non-surgical treatments do not ease your symptoms, your doctor may recommend a minor procedure called trigger finger release. This treatment helps free the trapped tendon so your finger can move smoothly again, reducing pain, stiffness, and locking.
During trigger finger release, your surgeon makes a small incision in your palm and carefully releases the tight pulley that is restricting tendon movement.
The procedure is usually done under local anaesthetic as a day procedure so that you can return home shortly afterwards. It typically takes 15 to 30 minutes, and you can start gently moving your finger soon after to prevent stiffness.
Also read: Recovering from Trigger Finger Operation
Recovery Expectations and Outcomes
Knowing what to expect after treatment can ease any anxiety you feel and help you plan your recovery.
Post-Treatment Hand Function and Follow-Up
After treatment — whether conservative or surgical — you can usually expect a gradual return of normal finger movement and strength, rather than an instant recovery.
If you are treated with splinting, medication, or steroid injections, improvement may begin within a few days to a few weeks. Stiffness and triggering often ease progressively, although full symptom relief can take several weeks. During this time, gentle finger exercises and activity modification help support recovery.
After trigger finger release surgery, many people notice immediate improvement in finger movement, especially reduced locking. However, mild swelling, tenderness, and stiffness are common in the early days.
You can usually start gentle movement on the same day or the day after surgery, with light daily activities resuming within a few days to one week. Grip strength and full comfort typically return within two to six weeks, depending on the healing and rehabilitation process.
Follow-up appointments allow your doctor to monitor healing, assess finger motion, and address any ongoing stiffness or discomfort. If you have diabetes, your recovery may take slightly longer, making consistent follow-up especially important.
Seek Orthopaedic Treatment for Trigger Finger
If you have diabetes and notice finger stiffness, clicking, or locking, don’t wait. Early assessment by an orthopaedic specialist can protect your hand function and improve long-term outcomes.
At Spire Orthopaedic, we provide personalised care to manage trigger finger and keep your hands moving comfortably.







